Radio Frequency Ablation
Radiofrequency ablation (RFA) is a medical procedure in which part of the electrical conduction system of the heart, tumor or other dysfunctional tissue is ablated using the heat generated from medium frequency alternating current (in the range of 350–500 kHz). RFA is generally conducted in the outpatient setting, using either local anesthetics or conscious sedation anesthesia. When it is delivered via catheter, it is called radiofrequency catheter ablation.
Two important advantages of radio frequency current (over previously used low frequency AC or pulses of DC) are that it does not directly stimulate nerves or heart muscle and therefore can often be used without the need for general anesthetic, and that it is very specific for treating the desired tissue without significant collateral damage.
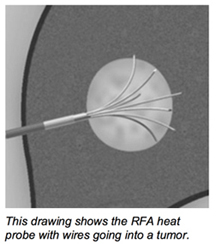
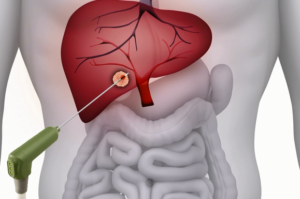
RFA may be performed to treat tumors in the lung, liver, kidney, and bone, as well as other body organs less commonly. Once the diagnosis of tumor is confirmed, a needle-like RFA probe is placed inside the tumor. The radiofrequency waves passing through the probe increase the temperature within tumor tissue and results in destruction of the tumor. RFA can be used with small tumors, whether these arose within the organ (primary tumors) or spread to the organ (metastases). The suitability of RFA for a particular tumor depends on multiple factors.
RFA can usually be administered as an outpatient procedure, though may at times require a brief hospital stay. RFA may be combined with locally delivered chemotherapy to treat hepatocellular carcinoma (primary liver cancer). A method currently in phase III trials uses the low-level heat (hyperthermia) created by the RFA probe to trigger release of concentrated chemotherapeutic drugs from heat-sensitive liposomes in the margins around the ablated tissue as a treatment for Hepatocellular carcinoma (HCC). Radiofrequency ablation is also used in pancreatic cancer and bile duct cancer.
RFA has become increasingly important in the care of benign bone tumors, most notably osteoid osteomas. Since the procedure was first introduced for the treatment of osteoid osteomas in the 1990s, it has been shown in numerous studies to be less invasive and expensive, to result in less bone destruction and to have equivalent safety and efficacy to surgical techniques, with 66 to 95% of people reporting freedom from symptoms. While initial success rates with RFA are high, symptom recurrence after RFA treatment has been reported, with some studies demonstrating a recurrence rate similar to that of surgical treatment. RFA is also increasingly used in the palliative treatment of painful metastatic bone disease in people who are not eligible or do not respond to traditional therapies (i.e. radiation therapy, chemotherapy, palliative surgery, bisphosphonates or analgesic medications).
Microwave Ablation
Microwave Ablation (MWA) is a form of thermal ablation used in interventional radiology to treat cancer. MWA uses electromagnetic waves in the microwave energy spectrum (300 MHz to 300 GHz) to produce tissue-heating effects. The oscillation of polar molecules produces frictional heating, ultimately generating tissue necrosis within solid tumors. It is generally used for the treatment and palliation of solid tumors in patients who are nonsurgical candidate.
MWA allows for flexible treatment approaches, including percutaneous, laparoscopic, and open surgical access. Therapy is generally performed with the patient under conscious sedation; however, in cases where intra-procedural pain is problematic a general anesthetic may be used. Ablations can be performed using a single MW antenna or a cluster of three to achieve a greater ablation volume. Tumor temperatures during ablation can be measured with a separate thermal couple; tumors are treated to over 60°C to achieve coagulation necrosis.
Trans- Arterial Chemo Embolization (TACE)
Trans catheter arterial chemoembolization (also called trans arterial chemoembolization or TACE) is a minimally invasive procedure performed in interventional radiology to restrict a tumor’s blood supply. Small embolic particles coated with chemotherapeutic drugs are injected selectively through a catheter into an artery directly supplying the tumor. These particles both block the blood supply and induce cytotoxicity, attacking the tumor in several ways.
TACE is an interventional radiology procedure performed in the angiography suite. The procedure involves gaining percutaneous transarterial access by the Seldinger technique to the hepatic artery with an arterial sheath, usually by puncturing the common femoral artery in the right groin and passing a catheter guided by a wire through the abdominal aorta, through the celiac trunk and common hepatic artery, and finally into the branch of the proper hepatic artery supplying the tumor. The interventional radiologist then performs a selective angiogram of the celiac trunk and possibly the superior mesenteric artery to identify the branches of the hepatic artery supplying the tumor(s) and threads smaller, more selective catheters into these branches. This is done to maximize the amount of the chemotherapeutic dose that is directed to the tumor and minimize the amount of the chemotherapeutic agent that could damage the normal liver tissue.
When a blood vessel supplying tumor has been selected, alternating aliquots of the chemotherapy dose and of embolic particles, or particles containing the chemotherapy agent, are injected through the catheter. The total chemotherapeutic dose may be given in one vessel’s distribution, or it may be divided among several vessels supplying the tumors.
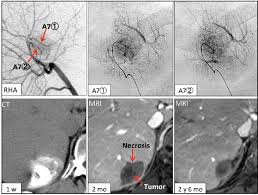
The physician removes the catheter and access sheath, applying pressure to the entry site to prevent bleeding. The patient must lie stationary for several hours after the procedure to allow the punctured artery to heal. The patient will often be kept overnight for observation and will likely be discharged the following day. The procedure is normally followed up with a CT scan several weeks later to check the response of the tumor to the procedure.
Other Radiological Procedure
We serve patients with some more radiological procedures such as PTBD, Fluid Aspiration. Please contact us for those procedures.
